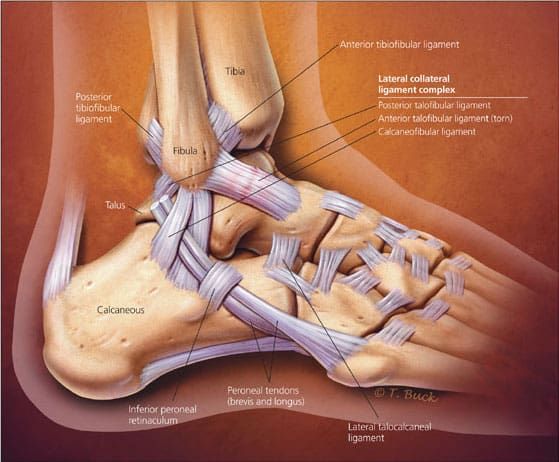
Anatomy of ankle ligaments
Ankle sprains are one of the most common musculoskeletal injuries seen around the world. The term ‘sprain’ is used frequently to describe a spectrum of injuries with varying severity. Typically an ankle sprain results in either a partial or complete tear of the supportive ligaments of the ankle joint.
The ankle joint itself is made up of the two bones in the lower leg (tibia and fibula) and the talus (large bone that connects to both the tibia and fibula). The joint is stabilised by surrounding ligaments that provide stability. These ligaments are comprised primarily of lateral (outer) sided ligaments and medial (inner) sided ligaments.
The lateral (outer) ligament complex is formed by three distinct ligaments.
- Anterior talofibular ligament (ATFL)
- Runs from the talus to the anterior (front) part of the tip of the fibula
- Calcanofibular ligament (CFL)
- Runs from the calcaneus (Heel bone) to the inferior tip of the fibula
- Posterior talofibular ligament (PTFL)
- Runs from the posterior (back) part of the talus to the posterior fibula.
The Medial (inner) ligament complex is called the ‘Deltoid‘ ligament. The deltoid ligament is a broad ligament with attachment from the lower part of the tibia (medial malleolus) and spans out to several of the small bones of the foot.
Ankle sprain – mechanism of injury
The majority of ankle sprain injuries occur following a twisting injury. Typically this is an ‘inversion’ type injury where the ankle turns inwards and the body ‘goes over’ the ankle joint. This pattern results in injury to the outer (lateral) sided ankle ligaments (ATFL / CFL).
There are varying degrees of severity of ankle sprains, depending upon whether the torn ligament/s is a partial or complete tear, and how many of the ligaments are involved.
Ankle Sprain – Making the diagnosis
Often a detail history is all that is needed to make the diagnosis of an unstable ankle joint. A patient who has had one or several ‘twisting’ ankle sprains, and who has the ongoing sensation that her ankle is going to collapse on them, has functional ankle instability.
A thorough examination is performed to not only assess the integrity of the ankle ligaments, but to also exclude any additional injuries to the surrounding cartilage and tendons.
A plain x-ray will assess for small bone fractures and any evidence of arthritis around the ankle joint.
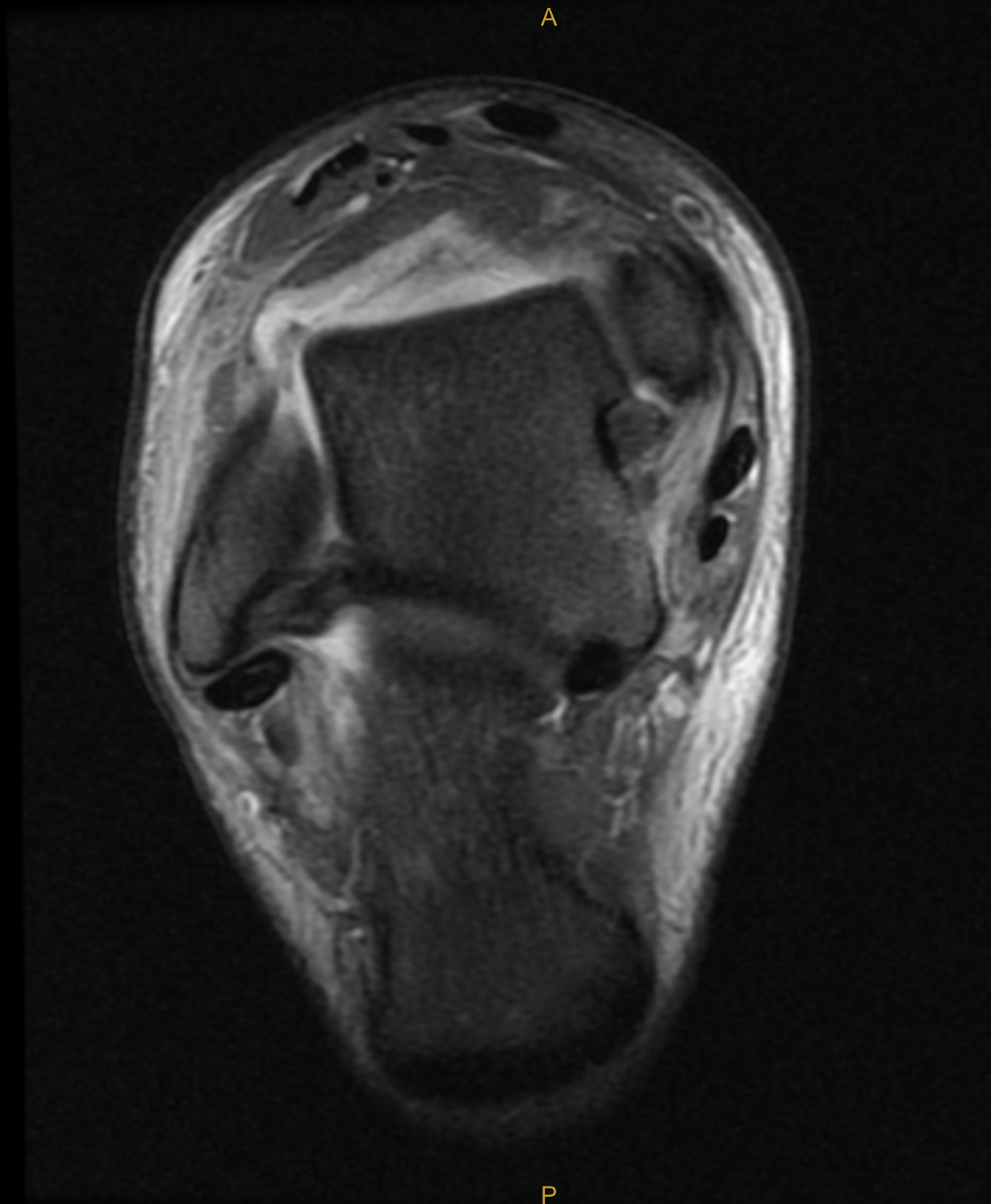
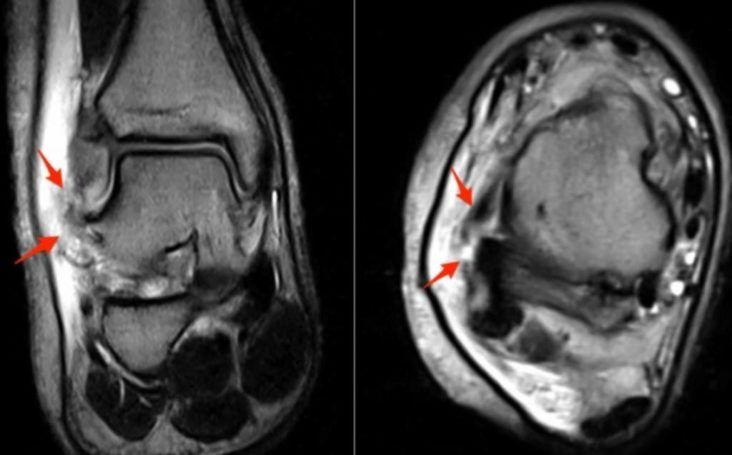
A MRI scan can give detailed information regarding the joint cartilage surface and the surrounding ligaments and tendons.
Ankle Sprain – Initial management
Up to 80% of ankle sprains heal well with conservative management. This treatment involves:
- Functional rehabilitation – Early mobility +/- a supportive orthosis.
- Gait retraining
- Proprioceptive training – i.e wobble board exercises to teach the ankle joint to stabilise itself
- Range of motion exercises – to reduce the risk of long term stiffness
- Peroneal muscle strengthening
Ankle sprain – When to consider surgery
Chronic ankle symptoms following an ankle sprain often include pain, instability (the feeling that the ankle joint is going to ‘roll over’), and persistent swelling. When any of these symptoms are present, despite conservative management, surgery is considered.
Patients who fail to recover from there original injury, warrant a review by an orthopaedic surgeon.
Causes of persistent pain may include:
- Ankle impingement
- Damage to the joint (cartilage) surface of the ankle joint
- A ‘missed’ fracture of one of the ankle/foot bones
- Injury to the supportive tendons of the ankle joint (i.e peroneal tendons)
- The development of arthritis within the ankle joint.
A loss of trust in the ankle joint and a feeling of ‘instability’ is another consideration for surgery to ‘tighten up’ the outer ligaments of the ankle.
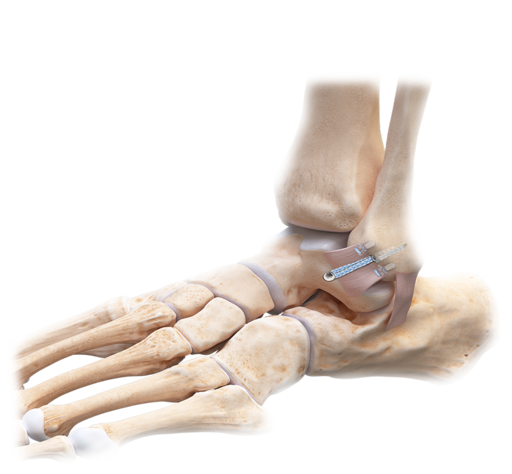
Ankle Ligament Stabilisation
Specialised sports reconstruction – Day Procedure
This technique is used to strengthen the outer (lateral) ligaments of your ankle joint. A keyhole arthroscopy is commonly performed at the same time to address any issues inside the ankle joint.
Do you experience any of the following?
Frequent Ankle Sprains
Pain in your ankle
Swelling around your ankle

